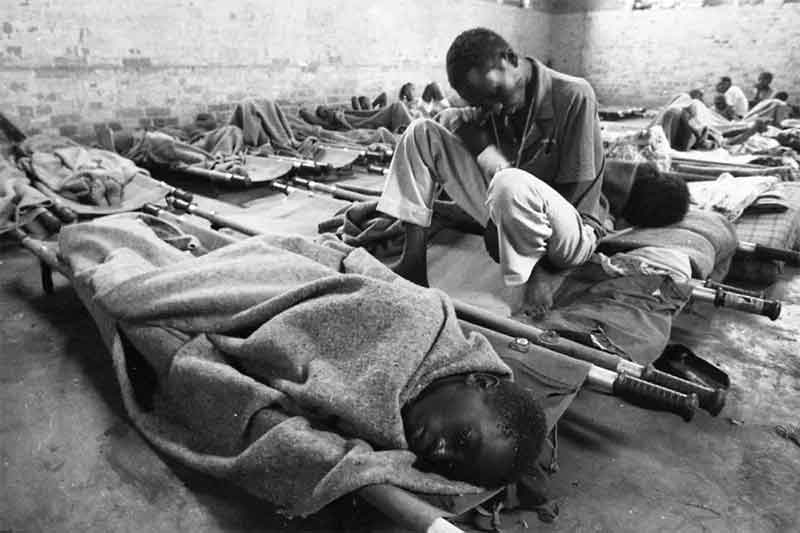
India’s economy is soaring but its healthcare system remains an Achilles’ heel. For millions of people, the high cost of treating illness continues to undermine economic progress. This is largely on account of the abysmal and chaotic healthcare system owing to the declining budgetary healthcare support by the government. India now ranks close to the bottom of the pile in international rankings on most health indices.
With an investment of 1.3% of GDP in health services— which has remained at the same level for a decade—India ranked 187th out of 194 countries according to the World Health Organization (WHO), while accounting for a full 20% of the global healthcare burden. Comparable rates are 1.5% in Sri Lanka, 2.7% in China, and 3% in Thailand. In order to remedy this, the National Health Policy 2017 has proposed an increase in public spending on health care from the current dismal rate of 1% to a meagre 2.5% of GDP by 2020. This would still leave India well below the world average of 5.99% of GDP.
Compared to its spending on health, India spends around 2.4% of its GDP on defence. Global evidence shows that, unless a country spends at least 5-6% of its GDP on health with most of that coming from public funds, basic healthcare needs are unlikely to be met.
Illnesses are a severe risk and can shave off most of the hard-earned savings in low income communities. They are the No. One route to bankruptcy. The Ministry of Health found that a quarter of all people hospitalised were driven to penury by their hospital costs ~ not including the cost of missed work.
Universal healthcare in India remains a distant reality because healthcare still continues to rank very low on the government’s priority card. Nobody wants to talk about the elephant in the room. While facilities in Indian metros are competing with the world’s best medical centres, the scenario beyond the urban conglomerates is quite distressing. The demand and supply in healthcare services still show a significant disparity in urban and rural areas as also regional imbalances. Here’s a snapshot:
- 30% of Indians do not have access to primary healthcare facilities.
- About 39 million Indians fall below the poverty line each year because of healthcare expenses.
- Around 30% of people in rural India do not visit hospitals due to fear of the expenses.
- 47% of healthcare needs in rural India and 31% of the need in urban areas are financed by loans or the one-off sale of assets
- About 70% of Indians spend all their income on healthcare and drugs.
- Out-of-pocket spending on healthcare in India—which makes up 69% of the total expenditure on health—is among the highest in the world, and is much more than the rates in Thailand (25%), China (44%), and Sri Lanka (55%).
Nearly 30,000 doctors, 20,000 dentists and 45,000 nurses graduate from medical colleges across India every year. However, the doctor-to-patient ratio in India is only six for every 10,000 people. This is far below the rate in Australia (1 for every 249), the UK (5 for every 1,665) and the US (9 for every 548). The global ratio stands at 15 doctors for every 10,000 people.
The distribution of doctors is also uneven across the country, with a low ratio in states like Chhattisgarh and Jharkhand—just two doctors for every 1, 00,000 people. And there are only six hospital beds and two surgeons per lakh of population. There is one government doctor for every 10,189 people, one government hospital bed for every 2,046 people and one state-run hospital for every 90,343 people. In comparison to these dismal numbers, the US has 24.5 doctors for every 10,000 people and one hospital bed for every 345 citizens.
India has a laggardly record in updating its healthcare coverage. In per capita terms, adjusted for purchasing power, India’s public expenditure on health is $43 a year, compared to $85 in Sri Lanka, $240 in China, and $265 in Thailand. European nations spend 10 times and the US 20 times. According to the Insurance Regulatory and Development Authority (IRDA), the Indian government’s contribution to health insurance stands at roughly 32%, as opposed to 83.5% in the UK. India’s high rate of out-of-pocket expenses for health in stems from the fact that 76% of Indians do not have any health insurance.
The recently released National Health Accounts (NHA) for 2014-15 show that the average amount spent by the government for each citizen per year was just Rs 1,108. This is against nearly Rs 6,300 spent on each central government employee. According to the NHA, India’s total health expenditure in 2014-15 worked out to Rs 3,826 per person. Of this, people had to spend Rs 2,394 (63%) out of their own pockets. In 2014-15, the Union government’s expenditure on the National Health Mission was Rs 20,199 crore. Spread this cash injection over a population of roughly 1.25 billion and it comes out to a paltry Rs 162 per head.
The apathy of the government is reflected in a rather poor prognosis for the health system. Primary health centres (PHC) in villages are supposed to screen and feed medical cases to specialised hospitals in districts and further on to state-level specialised hospitals. PHCs do not exist in many villages (about 1 for every 20 villages), and where present are so acutely undermanned that the “access” system is broken at the first mile. As many as 18 per cent of PHCs were entirely without doctors, This impacts not only the filtering of patients but also deeply impairs prevention and early detection which is a must if costs in the whole system are to be contained. The only redeeming feature is the committed cadre of Auxiliary Nurse Midwife (ANM) at PHCs and their sub-centres and accredited social health activists (ASHAs).
Our healthcare facilities have grown significantly in terms of numbers and expertise of our professionals, but this has largely been in the private sector. The government’s failure to deliver quality care has led to a rapid expansion of private hospitals, which today account for 93 per cent of all hospitals (up from 8 per cent in 1947), 64 per cent of all beds, and 80 to 85 per cent of all doctors. But mass access continues to remain a challenge. For the private sector, affordability in Tier 3 cities and rural areas is a critical limiting factor for further expansion.
The health infrastructure is heavily skewed in favour of urban areas. Nearly 75 per cent of dispensaries, 60 per cent of hospitals and 80 per cent of doctors are located in urban centres. Doctors cater to a third of the urban population, or no more than 442 million people.
There are around 734 district hospitals across the country which provide secondary healthcare facilities to people. In addition, there are around 300 other hospitals, such as women’s hospitals at the district level. They are powerful nodes in India’s healthcare network and can be revitalized to boost the health infrastructure.
India needs to reform the public health care sector’s governance and management systems. The approach to service delivery has to be a functional referral linkage and establishing a ‘continuum of care’ across the spectrum from village to sub-health centre to primary health care, sub-district hospital and the district hospitals. The challenge remains to reform the health system and its workforce in particular, so that practitioners, administrators and others have the skills, knowledge and professional attributes to meet the emerging health-care needs of our community.
Several laudatory policies are already in place. The direction of travel, so to speak, is right but we have to accelerate the pace of the journey. For reforms to be successful we need hard-coded timelines and accountability of those tasked with the administration. It is now for the policy doctors to collaborate with the professional doctors to use their ingenuity to come up with radical solutions that can cope with the mounting challenges of healthcare.
(Moin Qazi is the author of Village Diary of a Heretic Banker. He has spent more than three decades in the development sector.)