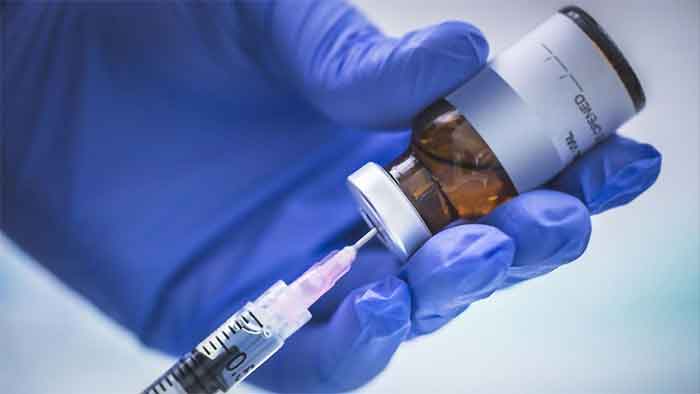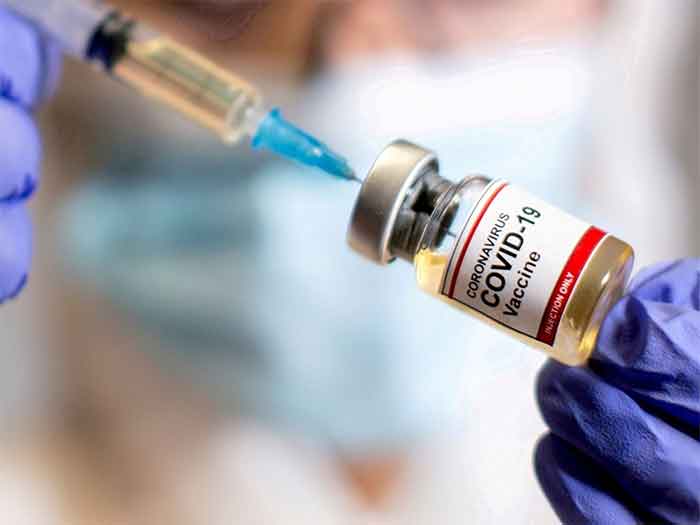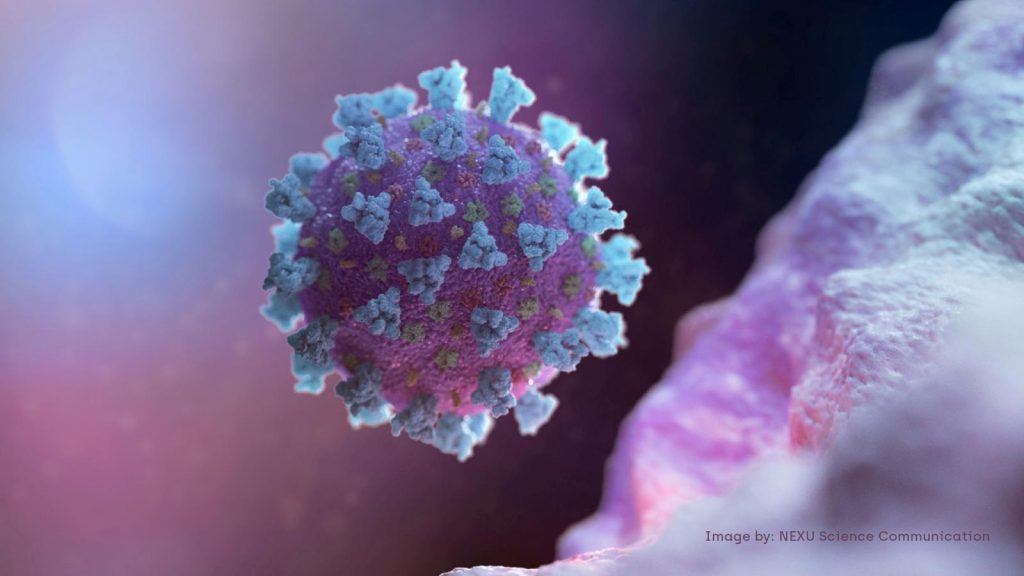
We are being told to wash our hands (for 20 seconds!) and self-isolate if sick. But what if you cannot do either of those things? One billion people live in slums or informal settlements where water for basic needs is in short supply – let alone 20 seconds worth – and where space is constrained and rooms are often shared. Yet discussion about vulnerability in these contexts has been startlingly absent, points out researcher Annie Wilkinson.
The medical industrial complex that dictates the health policies today has been exposed with the spread of the Carona virus, experts point out.
This complex, medical practitioners and the public need to recognise that health is not just an individual patient, doctor, hospital issue. There are wider socio economic and climate issues that affect health and which are being ignored, experts point out.
Today, worldwide, there is an apparent increase in many infectious diseases, including some newly-circulating ones (HIV/AIDS, hantavirus, hepatitis C, SARS, etc.). This reflects the combined impacts of rapid demographic, environmental, social, technological and other changes in our ways-of-living. Climate change will also affect infectious disease occurrence, the World Health Organisation points out.
Author and gastroenterologist Dr. Seamus O’Mahony challenges the usefulness and credibility of medical research; the illusion of progress; our stubborn belief that we can be perfected; over-prescribing; poly-prescribing; the efficacy of many drugs that are routinely administered; the corruption of academic medical research; our collective failure to accept that medicine cannot cure everything, and indeed can cause trouble of its own; over-reliance on metrics; the pharmaceutical industry and its vast reach and influence, and far more.
There was, he points out, a ‘Golden Age’ of medicine, from the 1930s to the 1980s, during which a number of huge advances were made. TB, smallpox, polio, all huge killers, were effectively eradicated in the developed world. This Golden Age has ended . There have been very big advances since then, but nothing like that accelerated level of discovery and innovation that occurred in those 50 years.” Since then, medicine has increasingly lost its way.
Many believed that medical research is being conducted in a coherent, structured, completely credible way, such that it will gradually solve all ills. That all one has to do is wait, and research will do the rest, finding cures for sicknesses long before we succumb to them. Maybe not, it seems. “Contemporary bio-medical research is itself very sick as an endeavour,” O’Mahony says. “There is even an acknowledgement and a consensus within bio-medical science that it has lost its way. It’s been estimated that anything up to 85pc of all bio-medical research is a waste of time. And that’s at a cost of $170bn (€150bn) annually.”
Even in the 19th century radical ideas on the subject emerged from FriedrichEngels and Rudolf Virchow. Engels called deaths caused by the system as social murders. I first heard of Virchow from Dr Binayak Sen. There is much more to health than hospitals and medicine. Socio-economic deprivation is the main problem. The focus has to begin from there. But we are obsessed with the corporate-medical industry syndrome.
In 1977 George Engel, a psychiatrist, psychoanalyst, and professor of medicine, published a paper in Science. It contained no data and, to be frank, it is rather dry read nowadays, but its 1600 citations have made it a classic. The main achievement of “The Need for a New Medical Model: a Challenge for Biomedicine”, was to put one word firmly into the medical literature: biopsychosocial.
Engel argued that an exclusively biomedical approach had left, “no room within its framework for the social, psychological, and behavioural dimensions of illness”, although nowadays the role of such factors in illness hardly seems contentious. Indeed, recognition of the role of social processes in disease goes back at least to Engel’s near namesake, Friedrich Engels, who in The Condition of the Working Class in England of 1845, described the appalling living conditions of the poor in rapidly industrialising England. Engels asked, “How is it possible, under such conditions, for the lower class to be healthy and long lived? What else can be expected than an excessive mortality, an unbroken series of epidemics, a progressive deterioration in the physique of the working population?” ts.
Ernst Bloch , the Marxist thinker, said all improvers of our situation who merely concentrate on health are so petit-bourgeois and odd, the raw fruit and vegetable brigade, the passionate herbivores, or even those who practice special breathing techniques. All this is a mockery compared with solid misery, compared with diseases which are produced not by weak flesh but by powerful hunger, not by faulty breathing but by dust, smoke, and lead. Of course there are people who breathe correctly, who combine a pleasant self-assurance with well-ventilated lungs and an upright torso which is flexible
Pritpal Timber, health professional, poins out that health is not produced by hospitals and the health system.Social determinants (wealth, housing, education, middle-class power, etc) are the main determinant of health. Health has been “expropriated” (Ivan Illich’s word) by the health system, which has wealth, power, knowledge, and methods and crucially “defines” what is health and how it should be measured.
Some people funding and running healthcare systems recognise the impotence of the systems when it comes to health as opposed to treating sickness and the capacity of health systems to swallow resources while producing ever less “value. So they create a façade of social health care which is very inadequate.
There is need to stress the importance of social and preventive medicine a subject ignored in medical colleges because of the bias of the powers that be. The whole system is so profit and money oriented that it is not bothered about this, nor about social and economic inequality that plays a big role in causing ill health.
Creative writers had a much better vision about health than some health professionals. Ibsen’s classic play Enemy of the People shows that environmental pollution is the main cause of the illness in the town in his play. The reformer who holds this point of view is treated as an enemy by vested interests. Similarly, Charles Dickens spent a lot of time in his prolific writing career to sanitary reforms in England.
Vidyadhar Date is a senior journalist and author of a book on democratisation of urban transport
SIGN UP FOR COUNTERCURRENTS DAILY NEWS LETTER