Co-Written by Dr. P.S. Sahni & Shobha Aggarwal
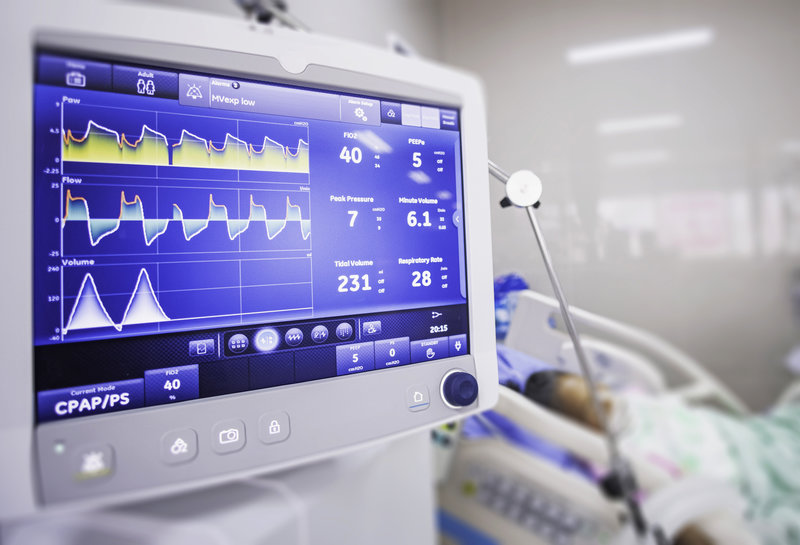
Governments all over the world – and not just in the developed west – are scrambling to get ventilators imported from the few countries which manufacture this machine e.g. China, Germany. The cost per piece is about Rs. five hundred thousand (Rs. 500,000)! The figure is about one and a half times the cost of by-pass surgery undertaken in heart attack patients in India. Sophisticated ventilators could cost up to Rs. 15,00,000 per piece. Media reports indicate that Indian government is shopping for 200,000 ventilators by June 2020!! This would entail an expenditure of Rs. 100,000,000,000 (Rs. One hundred billion) on the cheaper version to be imported.
USA has ordered 100,000 ventilators from Germany but the manufacturing firm indicated that it could send only 10,000 machines.
It is worth looking at the outcome of critically ill patients on ventilators being treated in Intensive Care Units (ICU); and how medical personnel – daring to care – in ICUs are themselves becoming infected with n-Coronavirus!
The International Edition of ‘The Guardian’, dated March 29, 2020 reported:
“Data from the Intensive Care National Audit and Research Centre (ICNARC) showed that of 165 patients treated in critical care in England, Wales and Northern Ireland since the end of February, 79 died, while 86 survived and were discharged. The figures were taken from an audit of 775 people who have been or are in critical care with the disease, across 285 intensive care units. The remaining 610 patients continue to receive intensive care.”
And that:
““The truth is that quite a lot of these individuals [in critical care] are going to die anyway and there is a fear that we are just ventilating them for the sake of it, for the sake of doing something for them, even though it won’t be effective. That’s a worry,” one doctor said.”
Worse still:
“Many of us (medical personnel) are also worried that we may be infected, yet asymptomatic (showing no symptoms) and therefore could be a potential risk to our patients, colleagues and families. That is the last thing that we would want, but we simply do not know.”
In a respected journal ‘The Lancet Respiratory Medicine’ published online February, 21, 2020 Xiaobo Yang and colleagues described 52 of 710 patients with confirmed COVID-19 admitted to an ICU in Wuhan, China. The ICU mortality rate was 79-86%. All 52 were adults.
A very high figure indeed.
The Times of India, April 1, 2020 (Page 9) presented the grimmest picture emerging from USA and Italy – the countries said to be having the best of medical facilities in the world. Just have a look:
“A supervisor urged surgeons at Columbia University Irving Medical Center in Manhattan to volunteer for the front lines because half the intensive-care staff had already been sickened by coronavirus. “ICU is EXPLODING,” she wrote in an email.”
And:
“Another doctor at a major New York City hospital described it as “a petri dish,” where more than 200 workers had fallen sick. Two nurses in city hospitals have died.”
Finally:
“Doctors and nurses fear they could be transmitting the virus to their patients, compounding the crisis by transforming hospitals into incubators for the virus. That has happened in Italy, in part because infected doctors struggle through their shifts, according to an article published by physicians at a hospital in Bergamo, a city in one of the hardest-hit regions.”
What is a ventilator?
To put it simply it is a device by which air/oxygen under pressure is pumped into a patient’s lungs when the latter is unable to breathe voluntarily in the normal way and is severely breathless. The device may be used for non-invasive ventilation at ICU admission through a mask on the patient’s face covering nose and mouth; or for invasive ventilation through a tube inserted into the trachea via the mouth or through a hole created surgically in the trachea. Split ventilators are available which could service 2-8 patients through just one machine (akin to split ACs). The air exhaled back by the patient could pose a risk to the ICU staff. This risk becomes manifold if high quality Personal Protection Equipment (PPE) is not available to the medical team; and also if negative pressure isolation room is not available in the hospitals; or if the ventilator is not equipped to ‘neutralise’ the exhaled virus. In the absence of these safeguards the fate of the ICU team all over the world (no exception) is not difficult to imagine.
In the context of COVID-19 pandemic do ventilators improve the over-all mortality rate of critically ill patients at a mass level in a country?
At a global level the overall mortality rate in n-Coronavirus is between 0-4%. In some countries this rate is more even with ventilators in use; whereas in some the figure is less even without ventilators or with a paucity of ventilators.
As data emerges from all the continents in the coming weeks and months one would get a fair idea on the usefulness or otherwise of ventilators. Even in ‘peace time’ i.e. when there is no epidemic around – the poorer sections of the society do not get access to ventilators particularly in developing/underdeveloped countries.
To define the role of ventilators a study along the following lines is in order:
Out of 10,000 patients who made it to ICUs each in USA/Italy/China during the COVID-19 pandemic what percentage died in spite of ventilator use? This should be compared with another 10,000 patients in three countries with poor health infrastructure where patients were not put on ventilators in hospitals/ICUs simply because ventilators were not available; what was the death rate amongst these patients? Do not be surprised with the results! Not a bit please.
To get an idea of what the results could be consider another common life-threatening disease – heart attack – where such studies have proved that at a mass level the morbidity and mortality rates are similar in the following two groups:
- those seemingly opting (read coerced) to get angiography, followed by angioplasty or by-pass surgery
And
- those ‘opting’ out of such investigations and surgery say due to non-availability of sophisticated health infra-structure in countries referred to – derogatorily – as under-developed. In such countries patients could make do equally well just by taking a few medicines daily.
Guess how long it took to get at these results – decades. Why? Well the vested interest of transnational corporations, funders for such studies, medical personnel, elected representatives, insurance companies reigns supreme. Worse, even now doctors worldwide continue with business as usual.
References:
- https://www.theguardian.com/society/2020/mar/28/coronavirus-intensive-care-uk-patients-50-per-cent-survival-rate
- Yang X , Yu Y, Xu J et al. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. Lancet Respir Med.2020; (published online Feb 21.) https://doi.org/10.1016/S2213-2600(20)30079-5
[Dr. P. S. Sahni & Shobha Aggarwal are members of AIDS Bhedbhav Virodhi Andolan (ABVA). Email: [email protected]]
SIGN UP FOR COUNTERCURRENTS DAILY NEWS LETTER









































