by Shobha Shukla & Bobby Ramakant

The year 2022 began on a dismal note, with its first week reporting the highest-ever number of COVID-19 cases in a week globally. Since the pandemic began in December 2019, the reported number of people who contracted the virus has been over 306 million and 5.5 million people have died due to it worldwide. The actual numbers could be much higher, as many infections and deaths are likely to have gone underreported.
Each of these infections could have been prevented, because we know how to prevent transmission of the SARS-CoV-2 virus. And had we prevented the spread of the infection, most of these untimely deaths could have been averted. But, alas, we are failing to break the chain of infection transmission.
The virus cannot multiply outside of living cells. Breaking the chain of infection transmission is still the golden cog-in-the-wheel for disease control. If we look at the weekly reports of the World Health Organization (WHO), the number of new infections has been consistently alarming, never dipping to the desirable zero. In fact, we saw the number of new infections peaking catastrophically on a few occasions, and/or in few geographical areas, or dipping or plateauing at times. Undeniably, since the pandemic began, one of the most important public health outcomes should have been achieving the target of zero new infections of the SARS-CoV-2 virus.
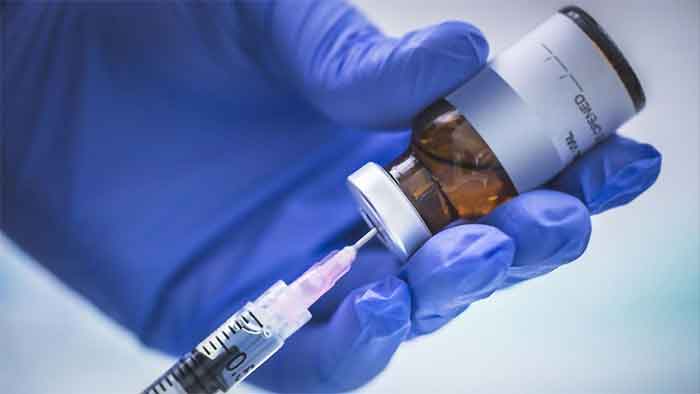
From very early in the pandemic, evidence-based ways to protect oneself from getting infected with the corona virus were widely popularized. Proper use of masks, maintaining physical distancing, frequent sanitising/ washing of hands, avoiding crowded places, preventing and managing co-morbidities that increase risk of serious outcomes of COVID-19, universal access to testing, and linking with clinical care pathways continue to be the best ways we can prevent the virus from spreading. Campaigns for SMSV – Social distancing, Masks, Sanitation and hygiene, and Vaccination, were robustly launched by People’s Health Organization led by infectious disease expert Dr Ishwar Gilada. Dr Gilada said to CNS (Citizen News Service) that SMSV campaign needs to be the central driver of COVID-19 responses worldwide.
Policies to support people in preventing diseases are key
“It is about making personal decisions for you and your family, and also having the policies to support you in those decisions to be able to keep yourself safe [from corona virus]. This is about distancing, keeping your distance from others outside of your immediate household, wearing of a well-fitting, appropriately-made mask” said Dr Maria Van Kerkhove, WHO Technical Lead for COVID-19 in a media briefing held recently.
She added: “When you put a mask on your face you need to have clean hands. It needs to cover your nose and your mouth. Wearing a mask below your nose, wearing a mask off your ear, wearing a mask below your chin is useless – it gives you a false sense of security that you have something on and it is protecting you but It will not.”
Individual actions are not enough to control the pandemic. That is why Dr Maria Van Kerkhove underlined “…we also need to make sure that there are national policies that support you in doing this: staying home if you are unwell, making sure that there are good testing facilities that are out there, and that people have access to reliable tests so that they know if they are infected and if they are infected to get into the clinical care pathway early because early clinical care saves lives.”
“We are asking governments to have rational, evidence-based, tailored, comprehensive policies with a layered approach of all of these different types of interventions that keep people safe. Just please be purposeful in what you are doing”, she said.
But some state governments in India have imposed night curfew, even though the WHO Chief Scientist Dr Soumya Swaminathan has said (as reported in the news) that “there is no science behind night curfews when it comes to tackling the spread of COVID-19 variants.” After all, major infection transmission is likely to happen during the social mixing and crowded places during the day. Merely imposing night curfew is not going to yield the desired public health outcomes. Dr Swaminathan added: “Politicians and policymakers need to start balancing the scientific and evidence-based methods we have to control COVID-19 transmission, to reduce its impact on people – particularly reducing deaths and hospitalisations, while at the same time, keeping economies open, making sure livelihoods are not impacted, because people have suffered enough.”
Omicron should not be categorised as mild
After undergoing 45 mutations, the corona virus has mutated into a smarter and more infectious variant- the Omicron. These mutations have made it easier for Omicron to infect human cells, have an immune escape so that fully vaccinated people, or those who have had COVID-19, are at risk of being (re)infected, and develop the ability to multiply in the cells of upper respiratory tract (instead of lower respiratory tract or lungs, as is the case with the previous variants).
“While Omicron does appear to be less severe compared to Delta, especially in those vaccinated, it does not mean it should be categorised as mild. Just like the previous variants, Omicron is hospitalising people and is killing people. In fact, the tsunami of cases is so huge and quick that it is overwhelming health systems around the world”, rightly said Dr Tedros Adhanom Ghebreyesus, WHO Director General.
Agrees Dr Maria van Kerkhove: “Hospitals are becoming overcrowded and understaffed, which further results in preventable deaths from not only COVID-19 but also from other diseases and injuries where patients cannot receive timely care.”
Omicron is not just more infectious in the community but also within households. Dr Michael Ryan, WHO Executive Director of Global Emergencies Programme said that studies done in the UK and South Africa, show that people in the household are at a 10% to 60% risk to contract omicron virus from a family member infected with the virus. However, those people who had been fully vaccinated had a much lower risk of having a secondary transmission in their household. Dr Ryan also highlights that we should “…recognise that the household is a place where you can reduce the risk of transmission.” It is our responsibility also to self-isolate if we feel sick, get tested, and as per the diagnosis, get appropriate treatment and care, without putting anyone else at risk of infection.
Let us hope that regardless of which variant has caused COVID-19, people with the disease may not need hospitalisation or die. While governments are scaling up vaccination against COVID-19, perhaps it is equally or more urgent to ensure universal adherence to basics of infection control. Breaking the chain of transmission of corona virus could be the gateway towards containing the pandemic.
We need to ensure that healthcare services for COVID-19 as well as for all other diseases that impact our populations are strengthened, not weakened. As there is no cure of COVID-19 as of now, the best shot to life we have right now is to protect ourselves from getting infected with the virus. More importantly, governments must ensure that policies and social supports are firmly in place for everyone, where no one is left behind, so that we all can break the chain of infection transmission.
(Shobha Shukla and Bobby Ramakant lead the editorial team at CNS (Citizen News Service). Follow them on Twitter @Shobha1Shukla and @BobbyRamakant)
Shared under Creative Commons (CC)