Written by Dr. Anamika Roy, Dr. Chandrima Chatterjee and Bhagyashree Dutta

Organ donation is the procedure of surgically removing an organ or tissue from one individual (the donor) and placing it into another individual (the recipient).[1] Transplantation is required when the recipient’s organ has failed or has been damaged by disease or injury. Organ transplantation is a major medical advancement. Organ donation and transplantation services portray a sub-system of modern healthcare organizations, which is a complex adaptive system.[2] However, number of people registering as donors are limited as compared to the number of people who require organ donation.[3] The outcome of organ transplantation requires the coordinated effort of many actors like donors, recipients, families, physicians, transplant coordinators and other hospital staff.[2]
The organs and tissues that are commonly indicated for transplantation are liver, kidney, pancreas, heart, lungs, intestine, cornea, middle ear, bone marrow, heart valves, connective tissue, etc.,[1]
Certain factors influence the process of organ donation, one of the important factors being a lack of knowledge about the transplant process and other being a deep distrust of the organ allocation system, and a belief in religious myths about organ donation.[4] These factors, while clearly affecting individual intentions regarding organ donation, may have an even more dramatic impact on the willingness to talk about organ donation with family members. Discussion about organ donation with family members is critical; without family consent, organ donation does not take place. It has been seen that knowledge is an important predictor of the willingness to talk about organ donation.[4] Thus, while many resources have been devoted to the creation of campaigns to increase the rate of individuals’ willingness to sign an organ donor card, these energies would be better spent understanding the variables that affect their willingness to talk about organ donation.
Sometimes there are potential taboos that might offend the family members while discussing about organ donation. This means that increasing general knowledge about organ donation (and reducing the myths about organ donation) is important to increasing the willingness of individuals to talk about organ donation with family members and to the lessening of resistance by family members to the desire of individuals to donate their own organs. This potential resistance on the part of family members is, in fact, a significant barrier to the willingness to donate organs.
Family communication and organ donation can therefore be described using an organ donation model. The ODM posits that the willingness to engage in family discussions is a function of the willingness to become a donor, which in turn is dependent on positive attitudes toward donation, a higher level of knowledge about donation, and positive social norms regarding organ donation. Nevertheless, the model does not account for the effect of less researched variables such as medical mistrust, bodily integrity, and religiosity.[4]
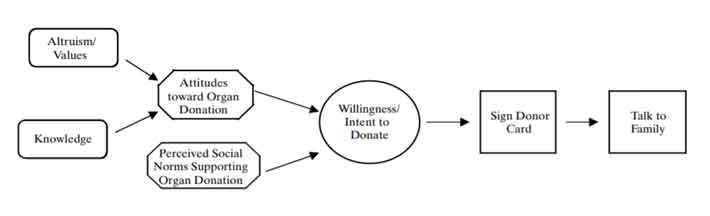
Studies reveal that people who are willing to talk to family members will be more willing to become potential organ donors. Secondly, attitudes toward family discussions about organ donation is correlated with higher levels of knowledge, favourable attitudes, and favourable social norms. Effective communication reported with higher levels of knowledge, favourable attitudes, and favourable social norms.[3][4]
Promoting family discussions about organ donation is vital to the process of organ donation. When family members know the wishes of their loved ones, they virtually always consent to donation. Conversely, the rate of donation drops precipitously when wishes of loved ones are not known. This means that understanding what factors contribute to family communication about organ donation, especially in a population with disproportionate needs for organ transplants, is at least as important as understanding the factors that contribute to individual decisions about becoming potential donors. Fortunately, this paper demonstrates that factors such as knowledge, attitudes, and social norms about organ donation contribute both to decisions about organ donation willingness and the willingness to talk to family members about organ donation.[3]
Dr. Anamika Roy is a dental surgeon and currently a postgraduate student, pursuing Master of Public Health (Health Policy) at Prasanna School of Public Health, Manipal Academy of Higher Education (MAHE), Manipal, India.
Dr. Chandrima Chatterjee is a dental surgeon and currently, a postgraduate student, pursuing Master of Public Health (Global Health) at Prasanna School of Public Health, Manipal Academy of Higher Education (MAHE), Manipal, India.
Bhagyashree Dutta is a physiotherapist and currently, a postgraduate student, pursuing Master of Public Health (Health Policy) at Prasanna School of Public Health, Manipal Academy of Higher Education (MAHE), Manipal, India.
References
- Cleveland clinic. Organ Donation and Transplantation. Retrieved from
https://my.clevelandclinic.org/health/articles/11750-organ-donation-and-transplantation
- Dhakate NN, Joshi R. Analysing Process of Organ Donation and Transplantation Services in India at Hospital Level: SAP-LAP Model. Global Journal of Flexible Systems Management. 2020 Dec;21(4):323-39.
- Murray L, Miller A, Dayoub C, Wakefield C, Homewood J. Communication, and consent: discussion and organ donation decisions for self and family. In Transplantation proceedings 2013 Jan 1 (Vol. 45, No. 1, pp. 10-12). Elsevier.
- Morgan SE. The power of talk: African Americans’ communication with family members about organ donation and its impact on the willingness to donate organs. Journal of Social and Personal Relationships. 2004 Feb;21(1):112-24.
GET COUNTERCURRENTS DAILY NEWSLETTER STRAIGHT TO YOUR INBOX