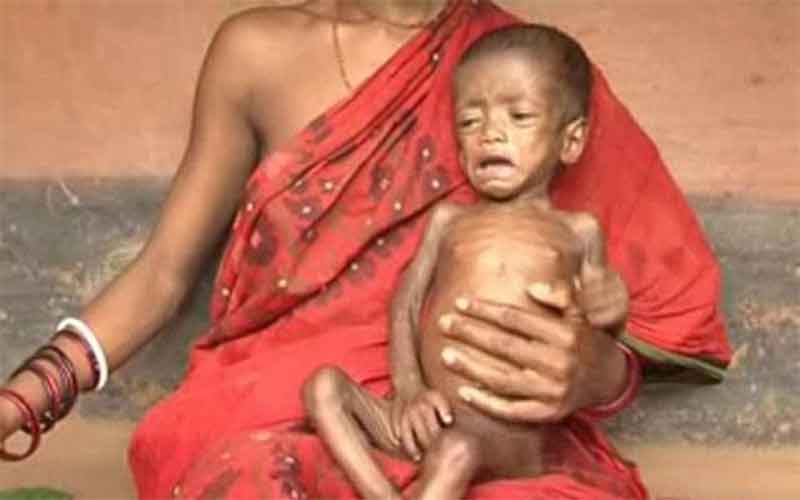
In Maharashtra, the administration has been claiming that there is a steady decline in the number of malnutrition and child deaths in the state. But, in recent figures that have come out, questions are being raised on the claims of the administration.
In the last 17 months, from January 2021 to May 2022, over 22,751 children in the age group of up to five years have died in the state according to a reply received to a Right to Information Act query by ‘Samarthan’, an organization working on children’s rights and health issues. Of these, 19, 673 were cases where the infant was stillborn.
As per the reply, Mumbai recorded the maximum deaths at 1,898, followed by 1,741 in Nagpur, 1,349 in Aurangabad, 1,127 in Nashik, 1,181 in Pune, 1,049 in Akola, 1,026 in Nandurbar and 1,015 in Thane.
 Sindhudurg district of Konkan region adjoining Goa has recorded the least number of deaths of 64 children. Similarly, in Washim district of Marathwada region, 89 children have died and 125 children have died in Latur district. Significantly, the more developed districts of the state account for 43 percent of the total child deaths in the state.
Sindhudurg district of Konkan region adjoining Goa has recorded the least number of deaths of 64 children. Similarly, in Washim district of Marathwada region, 89 children have died and 125 children have died in Latur district. Significantly, the more developed districts of the state account for 43 percent of the total child deaths in the state.
“The death of such a large number of children in a developed state like Maharashtra is worrying” says health activist Sudesh Patil.
Currently, there are over 12 state and central schemes being implemented to improve health conditions as well as reduce malnutrition and child mortality in Maharashtra. However, the increasing number of child deaths underlines the fact that these schemes are not having the positive and expected impact.
There are various causes of child mortality, but the factor of malnutrition is considered to be the most important at its root, hence there have been calls to form a special task force on this issue from Samarthan. According to the organisation the task force should include subject experts and representatives of social organizations. At the same time, Samarthan has also expressed the need to study the pattern of malnutrition in rural and urban areas.
The spike in stillbirths recorded in the last 17 months is believed to be due to the Covid pandemic. A recent study, conducted by the Indian Council of Medical Research (ICMR) and the National Institute of Research in Reproductive Health (NIRRH), found a higher frequency of severe Covid-19 and intensive care admissions among pregnant women and more maternal deaths between February and May 2021 compared with the same period in 2020.
According to UNICEF, in the last two decades India has reduced its stillbirth rate by 53% – from 29.6 per 1000 live births to 13.9 between 2000 and 2019. However, the pandemic threatens to reverse these gains.
The number of stillbirths among mothers infected with Covid-19 doubled during the second wave of the pandemic. According to UNICEF figures, there were 34 stillbirths per 1000 live births between February 2021 and May 2021 compared with the first wave that saw 15 per 1000 live births between April 2020 and January 2021. Both years the number of such deaths were significantly higher than the 13.9 recorded in 2019.
According to a global study published in JAMA Paediatrics in April this year, women with Covid-19 during pregnancy were 50% more likely to experience premature birth and pre-eclampsia, and require intensive care. The risk of maternal mortality was 22 times higher than those without Covid.
While the link between Covid infection and stillbirths is still being investigated the pandemic has certainly contributed by disrupting access to maternal care for pregnant women. It is believed that poor access to healthcare during the pandemic could have led to increases in stillbirth. WHO recommends at least eight prenatal check-ups, one ultrasound before 24 weeks of pregnancy, and daily intake of iron and folic acid supplements to prevent stillbirth.
All these were disrupted by lockdowns and the severe strain on the medical system. Several of the central and state government schemes for pregnant women that guarantee a minimum package of antenatal care services to women and access to nutrition were shut down during the pandemic period.
Another major factor behind increasing stillbirth cases has been the poor nutrition status of women due to loss of income of families. Over 77% of Indian households were consuming less food in 2020 during the pandemic and lockdown than before and food insecurity was higher among women, according to a report by Azim Premji University based on a survey on 5000 workers across the various sectors. Indian women’s dietary diversity declined during the lockdown of 2020 compared with the same period in 2019 showing decreased consumption of meat, eggs, vegetables, and fruit.
Apart from mothers, young children also have been deprived of regular nutrition during the Covid pandemic. At the national level, in November last year, the Ministry of Women and Child Development acknowledged that more than 33 lakh children in India were malnourished. More than half of these children were found to be in the severely malnourished category.
According to the report of the ministry, Maharashtra, Bihar and Gujarat top the states which have the highest number of malnourished children. Maharashtra recorded the highest number of malnourished children i.e. 6.16 lakh.
The problem is not confined to Maharashtra alone. According to the National Family Health Survey 2019-2021, there has been no significant improvement in health and nutrition status across India since 2015-2016. India has been ranked 101 out of 116 countries in the Global Hunger Index 2021, up from 94 in 2020.
Instead of calling social-welfare schemes ‘freebies’, as the Indian Prime Minister recently did, what many Indians need is even greater state investments to combat hunger and malnutrition – to save the lives of both unborn children and infants.
Shirish Khare has been associated with rural journalism for a long time and has been continuously reporting on the economic, social and health impacts of rural life during the Corona pandemic.