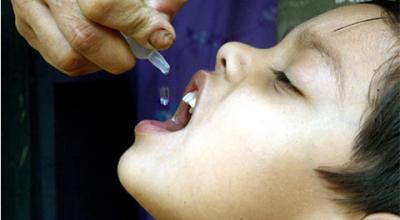
According to recent reports which have caused widespread concern, authorities in New York, London and Jerusalem have discovered evidence that polio is spreading there and the source of this has been traced to the oral vaccine itself. According to data quoted in a recent AP report ( Polio in US, UK and Israel shows rare risk of oral vax), since 2017, there have been 396 cases of polio caused by the wild virus, versus more than 2600 linked to the oral vaccine. This report also quoted Prof. Scott Barrett of Columbia University as stating, “We are basically replacing the wild virus with the virus in the vaccine which is now leading to new outbreaks.”
In order to place matters in perspective, it is also important to go back to several important but less known aspects of the polio eradication effort in India and some other middle and low income countries in the recent past. The polio eradication effort story in India and elsewhere has been widely promoted as a huge success-story but this has ignored several extremely important but less discussed aspects of this public health effort. Ignoring important aspects in the hurry to declare success can prove very costly as the necessary lessons are not drawn from costly mistakes and so such costly mistakes can continue to be repeated in future. In the interests of health and safety and for maintaining public trust in such public health efforts it is very important that a more comprehensive and realistic appraisal is placed before the people, an appraisal which should not try to avoid big mistakes that may have taken place but were clearly avoidable.
A fact of crucial importance that needs to be included in any realistic appraisal is that several hundred thousand children suffered attacks of even more deadly non-polio acute flaccid paralysis (NPAFP) as the pulse polio eradication campaign administered excessive doses. These afflictions increased after the entirely irrational introduction ( around year 2005 generally) of monovalent vaccine that contained 5 times the Type 1 viruses compared to the previously used vaccine. This tragedy-in-the-making was realized by health personnel in many countries and at the World Social Forum health summit a resolution was passed protesting against the high doses and introduction of monovalent type. Yet the tragedy continued.
Analyzing official data for India senior researchers found that in the period 2000-17 as many as 491000 children ( almost half a million ) suffered from NPAFP above the normal number of such cases. The maximum afflictions were in the states of Bihar and Uttar Pradesh. The year-by-year data is available in a widely discussed paper titled Corelation between Non-Polio Acute Flaccid Paralysis Rates with Pulse Polio Frequency in India published in the prestigious International Journal of Environment Research and Public Health. This paper was jointly authored by Rachana Dhiman, Sandeep C. Prakash, V. Sreenivas and Jacob Puliyel. The last mentioned senior doctor in particular has played an invaluable role in drawing attention to this and related issues.
In 2005 a fifth of the cases of NPAFP were followed up in Uttar Pradesh, a state of India, for 60 days by a highly reputed researcher Dr. Sathyamala. 35.2% were found to have residual paralysis and 8.5% had died. She examined data from the following year and found that children who were identified with NPAFP were at more than twice the risk of dying than those with wild polio infection.
The following resolution was passed by the ‘World Social Forum on Health’ and adopted by the WSF (World Social Forum) 2007, on the 24th of January, 2007 in Nairobi, Kenya.
“The II World Social Forum on Health condemns the World Health Organization’s lack of transparency in acknowledging the failure of the Global Polio Eradication Initiative strategy and instead,
(i) identifying a few low-income countries as scapegoats
(ii) subjecting the children of these countries to an unprecedentedly high number of Oral Polio Vaccine (OPV) through the pulse polio rounds with no concern for its negative impact and
(iii) the use of monovalent OPV, an untested vaccine without informed consent.
While the WSF on Health acknowledges the place of OPV in the overall immunisation programme as part of integrated public health services, the strategy of intensive pulse polio rounds has had a detrimental fragmenting effect on the already weak public health systems in low-income countries
We demand an independent review of the Global Polio Eradication strategy with due consideration to the relevant epidemiology and different countries’ health care priorities.”
In the course of the campaign for the eradication of polio complaints were increasingly heard in India ( and perhaps elsewhere too ) that excessive emphasis on this objective has reached such extreme levels that an adverse impact on other high priority objectives could be clearly seen. What is significant is that this criticism was also voiced in quite strong terms in an important official publication “Financing and Delivery of Health Care Services in India’ brought out by the National Commission on Macroeconomics and Health (NCMH) constituted by the Government of India.
In a background paper written by K. Sujatha Rao, the Secretary, NCMH, stated categorically, “The single-point pursuit of polio-eradication resulted in adversely affecting the routine immunization, which was initiated in 1986 as a Technology Mission for achieving full protection against all vaccine-preventable diseases by 2000. As per a household survey conducted in 1998 and again in 2003 (Indian Institute of Population Sciences 2004), the data for 220 districts showed that in the majority of the districts, there was either a declining performance or no improvement at all under the Universal Immunization Programme (UIP).”
Further this paper, written by none other than the Secretary of the Government constituted National Commission on Macroeconomics and Health, said, “Discussions with field staff seemed to suggest that this decline was largely on account of the emphasis given to polio, which not only commanded better resources and visibility in the media but also consumed nearly one-third of the time, 30 times the cost and exhausted the staff.”
This paper titled ‘Delivery of health services in the public sector’ recalled that in year 2003 the Government of India (GOI) had to dispatch half the departmental officials to oversee the Pulse Polio initiative (PPI) Round due to resistance from the local staff. The local staff had got tired of participating in 4 rounds of PPI (with each round requiring one whole month of preparation) as well as various other single-point campaigns, health melas of the GOI and family planning targets.
Ms. Sujatha Rao, who had access to a lot of authentic information, concluded, “Such isolated programmatic approaches have made it impossible to allow the health system to develop.” She raised a very pertinent question as to whether “vertically driven strategies implemented in a campaign mode, which are also resource intensive and neglect equally important public health functions, are worthwhile.”
Another paper, titled ‘Financing of Health in India’ drew attention to some dubious aspects of PPI. This paper has been co-authored by K. Sujatha Rao, S. Selvaraju, Somil Nagpal and S. Sakthivel of the Institute of Economic Growth, Delhi. Like the paper quoted earlier, this paper too is a background paper written for the National Commission on Macroeconomics and Health.
This paper informs us an estimated total of Rs. 3592 crores ( one crore=10 million) was spent on PPI during 1996-2005. This amount does not include the “extra-budgetary expenditures incurred by the WHO on the appointment of over 1000 consultants in the country to monitor the programme and the amounts being incurred by the UNICEF or IEC.” Almost 13% of the health department’s budget during 2003-04 was spent on this single activity. This paper adds, “It is estimated that one drop of polio vaccine is almost 30 times more than the drop given in routine UIP.”
Keeping in view these significant observations made on PPI in an important official document, which are also supported by many observations of senior health activists and doctors who have observed the reality of health programmes from close quarters, isn’t it time to have a second look at the Pulse Polio Initiative as well as other single-point campaigns and programmes which have been increasingly dominating our health system in recent years?
In particular a realistic appraisal of the polio control program is very badly needed. In the late 1980s when this program started at world level to eradicate poliomyelitis (polio), there were 350,000 cases in around 125 countries, affecting children under 5 years of age.1 in 200 infections led to irreversible paralysis. Among those who suffered paralysis, 5 to 10 per cent died. After 4 decades of this effort, polio elimination has been achieved to a large extent but it is still not complete, and the cases of vaccine related strains, which were recently reported to be higher than wild polio related cases, remain a cause of concern. But the bigger issue is that in the course of the eradication an extraordinarily high number of children suffered serious adverse consequences ( almost half a million in a single country India), some of them died, and this was a huge but avoidable tragedy. Warnings were given at a relatively early stage but ignored. Economic costs as well as costs to the health system were unduly high and could have been reduced significantly. If such costly mistakes continued to be disguised under a cloak of questionable success, then mistakes will continue to be repeated and those responsible for costly schemes will continue to have a free run.
Before concluding we will like to refer to a paper published in the Indian Journal of Medical Ethics ( April-June 2012). This paper titled ‘Declaring victory and moving on’ has been written by Dr. Neetu Vashisht and Dr. Jacob Puliyel. They write, “Clinically indistinguishable from polio but twice as deadly, the incidence of NPAFP was directly proportional to doses of oral polio vaccine received.” After showing why the goal of eradicating polio is not strictly achievable in scientific terms, this paper says that polio control based on routine immunization is a much better option than the excessive doses which proved very harmful. Hence the paper says that routine immunization must be strengthened, and perhaps one or two rounds of pulse polio may be needed. For this India should not depend on donors or imports but should create capacity to be entirely self-reliant in indigenous production and availability. The highly distorted program in India of excessive doses had started with a small foreign grant and ultimately India had to spend more than 100 times this amount on her own ( over 2.5 billion US dollars) while at the same time accepting the very wrong foreign advice for excessive doses which proved so harmful. Such glaring mistakes should not be repeated in future.
Bharat Dogra is Honorary Convener, Campaign to Save Earth Now. His recent books are Protecting Earth for Children, Planet in Peril and A Day in 2071.
















































