As on 6th August 2020, the coronavirus disease of 2019 (COVID-19) has affected 213 countries and territories around the world infecting over 19 million people of whom 0.7 million died. The US is on top with 5 million cases and 163,000 death. Brazil and India holds the second and third slots with 2.9 and 2 million cases. In terms of infection rates, Qatar, French Guyana and Bahrain hold the top three slots with 40, 27 and 25 cases per 1000 population. Infection rates in the US, Brazil and India are 15.0, 13.5 and 1.4 per 1000 people respectively (Worldometer). The SARS-Cov-2 emerged in Wuhan China sometime in November 2019. With city and province-wide lockdowns and community level actions like quarantine and social distancing, China has successfully controlled the epidemic in less than three months. Rest of the world is waiting for the vaccine.
As on 05 August 2020, there were 29,151 cases of Covid-19 in Kerala, the South-Western coastal State in India with a population 0f 35 million. Kerala’s infection rate is 0.81, which is lower than the national average. An earlier report in Countercurrents had reported the possible community transmission in a few places in Kerala. Further, a comparative study of Kerala and Washington States revealed different trajectories of the pandemic.
Report of the First 500 cases in Kerala.
The Government of Kerala has recently published the COVID 19 Clinical Management Report, a study of the first 500 persons with Covid-19 confirmed till 04 May 2020. Though clinical management reports have been published from other countries, this is the first of a kind from Kerala. After summarizing the main findings of the report, we will analyse the outcomes of all cases confirmed so far and compare it with other places and countries.
Asymptomatic Cases
Some infected people do not experience any symptom at all, throughout the course of infection. These persons are known as asymptomatic. The exact proportion of asymptomatic persons is not known. According to the current latest information, an asymptomatic person can also infect others. China started reporting the number of asymptomatic cases only since March 2020, when the epidemic was almost under control. Daily situation reports published by the WHO and the European Centre for Disease Control (ECDC) do not show the number of asymptomatic. Globally, sample surveys are the only sources of information on this group.
Among the 500 cases included in the GoK Report, 210 persons, 42% of the caseload remained asymptomatic throughout the course of infection, lasting for about ten days. All the 500 persons were admitted to the covid-care hospitals and discharged only after their swab tests were found negative for the virus.
According to a WHO review dated 27 Jul 2020, the proportion of truly asymptomatic cases ranges from 6% to 41%, with a pooled estimate of 16%. Among the limitations of the studies in this review were (a) some studies did not clearly describe how they followed up with persons who were asymptomatic at the time of testing to ascertain if they ever developed symptoms, and (b) others defined “asymptomatic” very narrowly as persons who never developed fever or respiratory symptoms, rather than as those who did not develop any symptoms at all. The WHO also mentioned a recent study from China that “clearly and appropriately defined asymptomatic infections, which suggested that the proportion of infected people who never developed symptoms was 23%”.
Lungs of the Asymptomatic
The GoK report quotes data on asymptomatic persons from a review paper published in the Annals of Internal Medicine, in which 6% to 95% of the caseloads were asymptomatic. Many of those asymptomatic persons became symptomatic few days after the tests. Shohei Inui and colleagues conducted a follow-up study of asymptomatic Japanese citizens confined in the Diamond Prince Cruise ship, which was published on 17 March 2020. In the CT-scans, they found lesions consistent with inflammation of the lung tissue (jargon – ground-glass opacities), in 54% of the cases. Referring to this and another study from S Korea, Daniel P. Oran and Eric J. Topol at the Scripps Research Translational Institute wrote in a commentary in the Washington Post on 11 June 2020:
“The lungs of asymptomatic people were found to have abnormalities that have become a well-known sign of covid-19. It is not clear what these lung abnormalities might mean for the long-term health of the asymptomatic — a stark reminder that science is only now beginning to understand the multiple ways that this novel pathogen can harm people.”
The asymptomatic Covid-19 cases included in the GoK study, scored more than 2,000 patient days in hospitals. It appears that they were not subjected to CT scans or other routine laboratory investigations. As of now, there are over 4,000 asymptomatic cases in hospitals in Kerala.
Symptoms of patients in Kerala and China
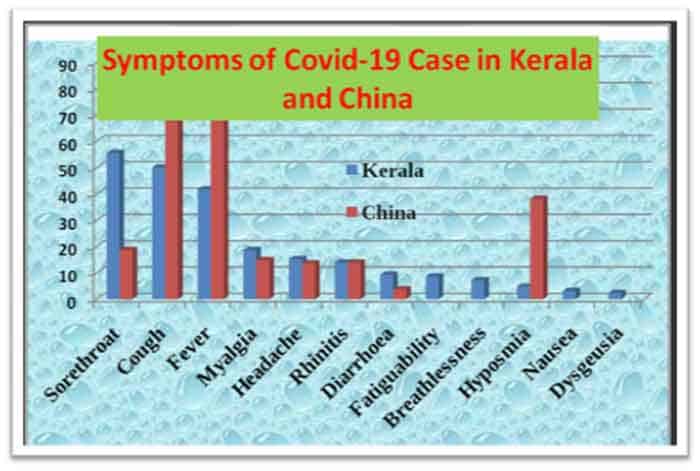
In Kerala, sore throat was the most reported symptom (56%), followed by cough (50%), fever (42%) and myalgia -muscle pain (19%). In contrast, fever (88%) and cough (68%) were the most reported symptoms in China and also in other countries, for which analyses are readily available. In Kerala 9% of the patients reported diarrhoea which was three times larger than that in China. At the same time, 38% of the patients in China experienced difficulty in detecting odour (hyposmia), which was 2.8% in Kerala. In Kerala, 7 patients (1.4%) also reported distortion of the sense of taste (dysguesia). The graph 1 below gives details of symptoms reported from Kerala and China.
Severity of Covid-19 – Kerala and other countries
In the GoK Report, the asymptomatic persons are also included in the group of patients with mild severity. I have excluded the asymptomatic group from the severity classification, in line with the global practice. Out of 290 patients with symptoms in Kerala, 54% were mild, 39% were moderate and 7% was severe. Graph 2 compares the severity of Covid-19 in Kerala with other places.
The data for Europe is extracted from ECDC’s Surveillance Report for cases in the European Union and the United Kingdom. The Wuhan data are available in a paper published by Pen et al in the Journal of American Medical Association. WHO data is extracted from a document dated 27 May 2020.
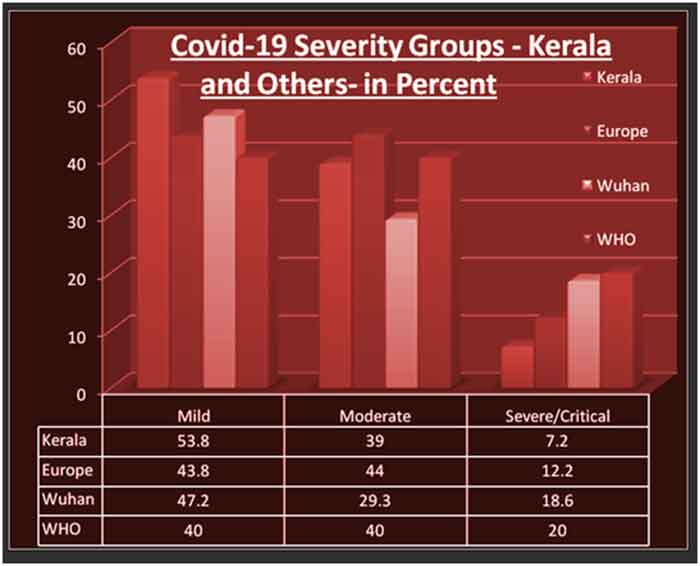
Kerala state has the highest proportion of mild cases and the lowest proportion of severe cases.
Co-morbidity and Hospitalisations
While the virus can infect any person irrespective of age or sex or race, the outcomes like severity of the disease, hospitalization, admission to intensive care unit and recovery or death is to a large extent determined by co-morbidity or underlying conditions.
In Kerala, 11% of the patients reported co-morbidities like diabetes, bronchial asthma, heart and kidney disease, cancer etc. The percentages of patients with co-morbidities in China, Europe and USA were 26, 46 and 76 respectively. The GoK does not provide the data on smoking which was found to be an independent risk factor in other studies.
In Kerala, all the patients and the asymptomatic persons were hospitalized. The mean of number of days from symptom onset to swab collection and hospitalisation in Kerala is 1.7 and 3 days respectively.
In the countries under comparison, asymptomatic persons and patients with mild symptoms were not hospitalized. The rate hospitalization in China, Europe and USA are 11, 32 and 25 percents of the confirmed cases respectively. The rates of co-morbidity and admission among the confirmed Covid-19 cases in China, Europe, US and Kerala are given in graph No 3. The total numbers of patients included in the studies in the graph are China -20812, Europe -95645 and US– 10647.
In Wuhan, where the epidemic surfaced during the middle of December 2019, there was a delay of one-to two weeks between the appearance of the first symptom and hospitalisation till the second week of February 2020.
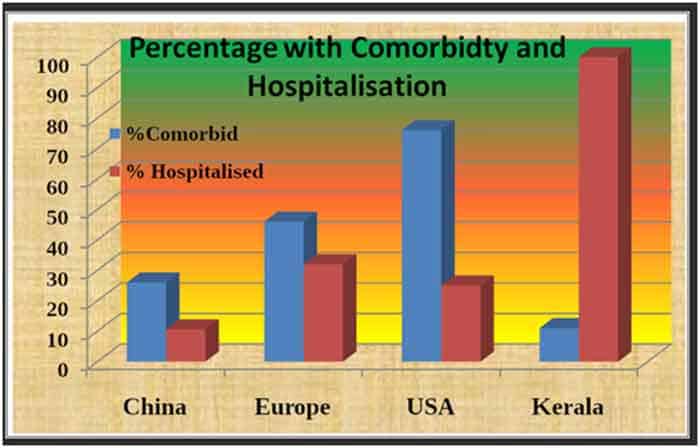
Attributes of the First Five Hundred Cases
Median age of all patients in Kerala was 35 years. The group with moderate symptoms had the lowest median age, while the severe patients scored the highest. The asymptomatic persons spent on an average 9 days in the hospitals. The hospital stay was longer for the symptomatic group. While the asymptomatic cases were virus positive for 9 days, there was a severity dependent increase among the symptomatic groups. Details are in Graph No 4 below:
According to the WHO review mentioned above, “the duration of RT-PCR positivity generally appears to be 1-2 weeks for asymptomatic persons, and up to 3 weeks or more for patients with mild to moderate disease, and much longer in patients with severe disease. This assessment is in line with the findings from Kerala.
Sex Ratio
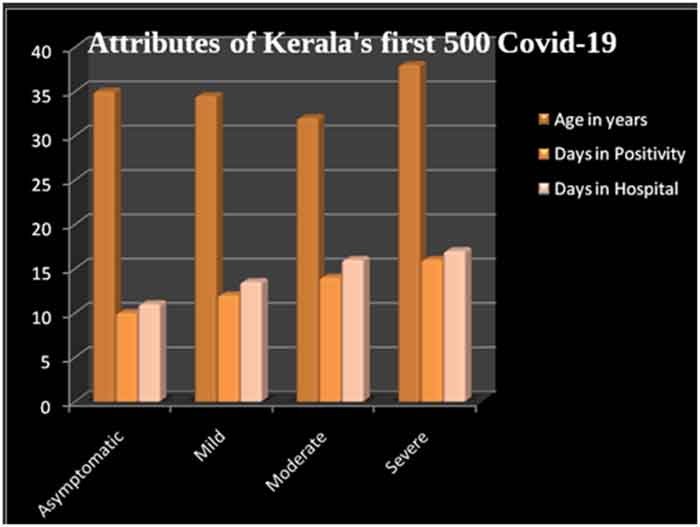
According to GoK Report, only one-fourth of the total caseload in Kerala is women; the sex ratio- SR- (males per 1000 females) is 3,257. During the first phase of the epidemic, majority of the infected persons were travellers, which explains the high male excess. This anomaly is getting corrected as more and more non-travellers also get infected.
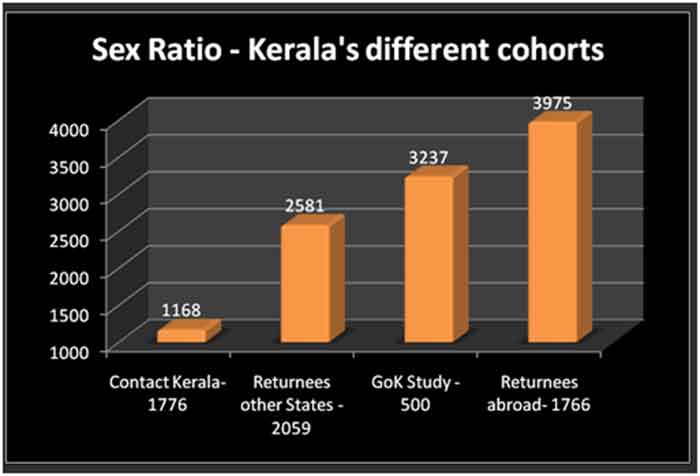
To know the trend, I have grouped the Kerala caseload into three cohorts – (a) Contacts – consisting of infected persons without travel history, (b) returnees from other Indian States (c) returnees from abroad. This analysis is based on the sex-disaggregated data tracked by a voluntary group – covid19kerala.info from the daily outbreak reports from the Government. Sex Ratio (SR) among three cohorts and te GoK report is shown in Graph below. The sample sizes of the cohorts are given in the axis labels. As expected, there is high male excess among the travellers.
Hydroxychloroquin trial
The GoK Report says that “the early administration of hydroxychloroquine (HCQ)+Azithromycin to this high risk groups (moderate to severe patients) may be a factor preventing progression from mild to moderate-severe disease in critically ill. This hypothesis however has to be validated by analysis data from a larger number of patients. Elsewhere in the report, it is mentioned that 90 patients (18% of the hospitalised persons) were administered HCQ. The number of patients who received the combination of HCQS+Azithromycin is not stated.
The GoK report is undated, it was finalized on 25 June 2020 or later.
On 17 June 2020, WHO announced that the “HCQ arm of the Solidarity Trial to find an effective COVID-19 treatment was being stopped, based on evidence from the Solidarity trial, UK’s Recovery trial and a Cochrane review of other evidence on HCQ. Data from Solidarity (including the French Discovery trial data) and the recently announced results from the UK’s Recovery trial both showed that hydroxychloroquine does not result in the reduction of mortality of hospitalised COVID-19 patients, when compared with standard of care.”
Case fatality Rate in Kerala
According to the GoK Report, there were 3 deaths among Kerala’s first 500 confirmed cases. Out of the three, one was an infant with congenital heart disease; the other two also had co-morbidities. The Case fatality Rate (CFR), defined here as percentage of dead among the total patients is 0.6%.
As of 06 August 2020, there were 29,151 confirmed cases and 94 deaths in Kerala. The death rate during the whole period is 0.31%. Globally, the CFR of Covid-19 ranges from 0.1% to 16.1%. Here, we will compare the CFR of Kerala and other places.
CFR for India is 2.1%, which is 7 times higher than that of Kerala. Such inter-regional differences have been seen in other countries as well. For instance, Wuhan a city of 11 million in China had a CFR of 7%, as against 3.5% in Hubei Province less Wuhan and 0.7% in 30 provinces of Mainland China less Hue=bei. The CFRs for Kerala, India, Wuhan and China are shown separately without any geo-political intentions.
Source of data
The data for Kerala is from the GoK dashboard. The data for Wuhan and China are extracted from the situation reports of the Hubei Health Commission and the CDC China for 24 May 2020. Rest of the data is extracted from the Worldometer. ((for 02 August 2020)
The graph 6 below shows CFR of Kerala, India, Wuhan and other places.
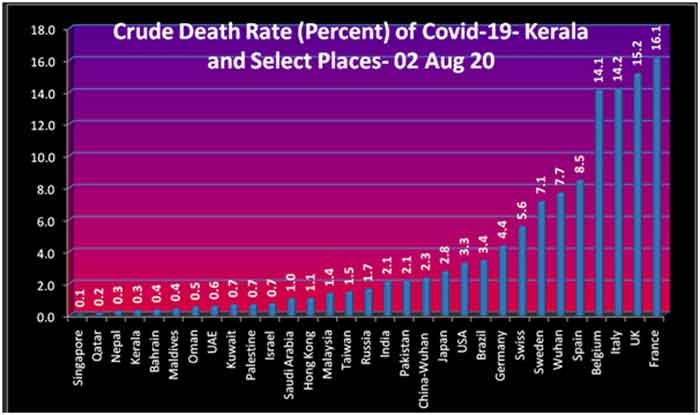
Singapore and Qatar, which have the lowest CFR are city-states with no rural population. Nepal, which is predominantly rural and Kerala which is partly rural and partly urban come next.
The GoK study reveals that the severity distribution, co-morbidities, a large number of asymptomatic in the caseload of Kerala. More importantly the age structure of the cases and the decadents are grossly different from that of China, Europe or America. (This issue will be discussed in detail in the next chapter).
The Kerala’s Covid-19 Control and Prevention work has been praised by the WHO, major science journals and the global media. Ms Payden, Acting WHO Representative to India said that Kerala’s “template could serve as a great example for other states to emulate”. About more than 95% of the Kerala’s Covid-19 team in the State are women and the team is led by two wonderful women, Smt. K.K. Shylaja Teacher Minister for Health & Social Justice and Dr. Sarita.R.L. the Director of Health Services. By providing sex-disaggregated data of Covid-19, Kerala can again become a model for other Indian States and also countries like the US
SARS-Cov-2 established its habitat among the humans some 10-11 months ago. Is it now a single entity or are there several landraces in different regional and geographic settings? This issue will be the focus of the next report.
VT Padmanabhan is an epidemiologist. He conducted genetic epidemiological and occupation health studies among people living in high background radiation areas of Kerala, among the workers of the Indian Rare Earths and Gwalior Rayons in Nagda, Madhyapradesh and the survivors of gas leak at the Union Carbide (now DOW chemicals) plant at Bhopal.
SIGN UP FOR COUNTERCURRENTS DAILY NEWSLETTER